
Sustained, bad occupational posture or habitual wrong posture of the neck in relation to the thoracic spine and shoulder joints results in stretching of the soft tissues on one side and elongation or lengthening of the ones on the opposite side. This can cause irritation and strain of the ligaments, muscles or joints precipitating cervical pain.

If you spend several hours a day working on a computer, you may unconsciously find yourself adopting poor postural habits, such as hunching over your keyboard. This position is usually a sign that you have a tight chest and a weak upper back. Over time, this type of posture can contribute to you developing a rounded upper back, a condition called kyphosis, which can cause shoulder and upper back stiffness and pain. When hunching over a computer, your head may tend to lean forward, which can cause stiffness and pain in the neck. Mobile device usage can also encourage you to hang your head and can cause similar problems dubbed "text neck". Upper back, neck and rear shoulder strengthening exercises, chest stretches and neck posture drills are recommended to help correct a hunched back.

Stand with your back against a wall. Place your arms against the wall so that the back of your hands touch the wall and are at the same height as your head. In this position, your elbows should be bent and held about six inches away from your waist. Raise your arms up above your head as far as you can reach while keeping your back and arms against the wall. As you raise your arms, push your shoulder blades into the wall. Pause at the top and then slowly lower back down to the starting position. Repeat 15 times. This stretch also targets the pectoralis major and subscapularis muscles.

Many people poke their chin forward to look up at a computer screen or TV when sitting without realising it. The poking chin posture is often caused by sitting too low, a screen set too high, a hunched back or a combination of all three. An unsupported lower back or a hunched upper back both encourage the neck to lean and tip the head downward. To compensate for this downward pressure, we lift the chin to look forward without straightening the back. A poking chin posture can lead to muscle weakness around the neck, compressing the neck joints, which over time can lead to stiffness and pain in the neck, shoulders and upper back and cause headaches. Correcting a poking chin involves improving your sitting habits and exercises to correct your posture.
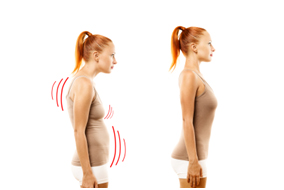
Most people stand with their round shoulder or hunch back. This is very poor posture as you are using too many muscles to hold straight up, & get easily fatigue. The cause of your round back is an imbalance of chest muscles. The chest muscles are too tight & back muscles are too weak.
Kyphosis, also known as a round back or hunchback, is a condition in which the spine in the upper back has an excessive curvature. The upper back, or thoracic region of the spine, is supposed to have a slight natural curve. The spine naturally curves in the neck, upper back, and lower back to help absorb shock and support the weight of the head. Kyphosis occurs when this natural arch is larger than normal.If you have kyphosis, you may have a visible hump on your upper back. From the side, your upper back may be noticeably rounded or protruding. In addition, people with hunchback appear to be slouching and have noticeable rounding of the shoulders. Kyphosis can lead to excess pressure on the spine, causing pain. It may also cause breathing difficulties due to pressure put on the lungs. Kyphosis in elderly women is known as dowager’s hump.
Kyphosis is a primary curvature & secondary curvature developed later. However, it rarely occurs in newborns because it is usually caused by poor posture. . Kyphosis can affect people of any age. Kyphosis caused by poor posture is called postural kyphosis.
Much of our flexibility, mobility, and activity depend on the health of the spine. Getting treatment to help correct the curvature may help you reduce the risk of complications later in life, such as arthritis and back pain.
Treatment for kyphosis will depend on its severity and underlying cause. In the case of Scheuermann’s disease, a child may receive physical therapy, braces, or corrective surgery. In cases of infection, patients take antibiotics. In cases of tumors, surgical removal is likely. For osteoporosis, it may be helpful to treat the bone deterioration to prevent kyphosis from worsening. For kyphosis caused by poor posture, you will not need aggressive treatments. However, the following will help relieve the symptoms of kyphosis:
For most people, kyphosis does not cause serious health problems. This is dependent on the cause of the kyphosis, however. If kyphosis is caused by poor posture, you may suffer from pain and breathing difficulties. These will only get worse later in life. Treating kyphosis early by strengthening the muscles of the back, seeing a physical therapist, or receiving chiropractic adjustments may be helpful. To decrease pain and other symptoms, the goal will be to improve your posture long-term.


SIT UP STRAIGHT AS MUCH AS POSSIBLE. OTHERWISE THIS posture MAY INCLUDE IN YOUR HABIT. And because of habit, lumber curvature may convert in to straight spine or lumber khyphotic. It may be postural or later structural deformity. Because of this posture many problems attack on your body. For e.g; back pain, legs pain, numbness or radiating pain in to legs due to disc pressure on the nerve root, stiffness in shoulders and neck and may affect standing or walking posture.
Back pain can indicate a serious condition and can be accompanied by other symptoms such as unintentional weight loss, pain that worsens at night and does not resolve with rest, bladder or bowel incontinence, and weakness in the hands and/or feet. It is important for patients to tell their health care professional about all occurring symptoms.
The goal of treatments for low back pain is to reduce pain and restore function, strength, and prevent injury reoccurrence. A combination of treatment may be recommended by your health care professional. In a few serious cases, surgery may be performed to relieve low back pain.

First you stand in anatomical position, straight forward, looking ahead parallel to the eyes. Lift up your arms together up to 160 to 180 degree, and then gradually stretch up your body until you feel increase the curve of lumber. Hold 10 to 20 second. Then, come to the normal position. First loose your body then keeps down your arms slowly & takes rest until you feel relax. Note- Repeat it this posture 5 to 10 times. Remember, your head should not forward or backward,
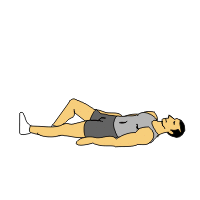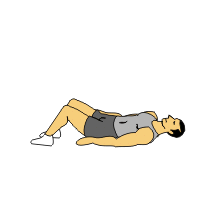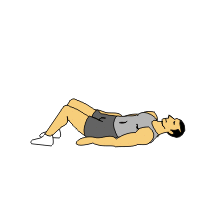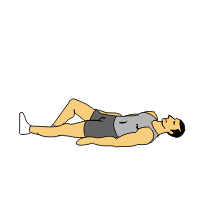
Lie on your back on the flat surface with knee bent and your feet on the floor. Keep your arms by the side of body with palm downward and head should not be raise. Now Raise your forelegs together up to 70 to 90 degree and hold 10 t0 20 seconds and repeat 5 to 10 times. Your pelvic should not be move.

This is called BRIDGING exercise.(strengthen core muscles) In starting position, lie on the flat surface with knees bent; place your hand at your side. Your shoulders & neck should be on the surface in relaxing position. Exercise position- gradually lift up your hips of the floor until your hips are aligned with your knees & shoulder. Hold 10 to 20 second and keep down slowly. Repeat 5 to 10 times.

Lie on your stomach face down and your palms flat on the floor. (1st position) >Keep your pelvis on the floor, Lift your self up onto your elbows. (2nd position) Raise your chest and allow your lower back to sag and lengthen. (3rd position) Look straight ahead don’t arch your neck by looking up. Hold this posture for 5 to 10 seconds relax and repeat 10 to 20 seconds. Raise your chest and allow your elbows straighten and rest the pelvis on the floor.(4th position hyper extension of lower back)

First you go in quadruped position. Body weight lies on the knee and palms with straight elbows. Raise your arm of one side and leg opposite side. Means right arm and left leg. Head and neck should be in neutral position. Hold 10 to 20 seconds and same do for other side. Repeat 5 to 10 times.Alert – The reasons of back pain may be different. Spinal extension movements are restricted, If some one having severe problem of the spine due to backward spoldylolisthesis or spinal canal stenosis ,or acute vertebral fracture;

When we stand normally or working in standing position for prolong time, unknowingly our body weight tends to lies on the one leg & second leg take rest without bearing weight. Because of this position, the pressure of body weight comes on the weight bearing joints of one le. Pelvic tilt latterly and disrupted of spine curvature. Whenever this posture is included in the habits, we get pain in to back, hip joint, Sacroiliac joints, knee or ankle joint.
The lateral pelvic tilt is a postural deviation in which one side of your pelvis is tilted to your left or right, causing one side of your hip to appear higher than the opposite side. This can cause the shoulder on the same side or the opposite side of the higher hip to elevate, resulting in back and hip pain and movement dysfunctions. Corrective exercises can improve your posture by addressing the cause of the postural deviation rather than the symptoms of the deviation.
This exercise works on stretching and moving the muscles and fasciae that connect your pelvis to your spine, shoulders and limbs. You may find one side of your body move better than the other side. Lie on the ground on your back with your arms straight on the ground near your head and your legs slightly apart. Reach your left hand and right foot away from your body with your right heel pushing away. Hold this stretch for three deep breaths and reach with your opposite limbs. Perform two sets of 10 reps on each side of your body.


Like the previous exercise, this also elicits the same benefits; however, the prone position places less stress upon your lower back. Lie on the ground on your stomach with your legs slightly apart. Bring your arms near your head with your palms facing down so that your head is between your biceps. Put a small towel beneath your face to cushion your forehead. Reach your left hand and your right leg away from your body. Hold this stretch for three deep breaths and reach with your opposite limbs. Perform two sets of 10 reps on each side of your body.
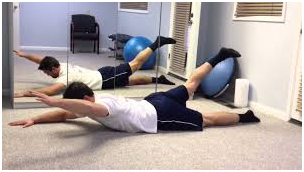
This exercise stretches the muscles and fasciae along the side of your pelvis, torso and shoulder while keeping your lower body stable in the kneeling position. Kneel on the ground on your right knee with your left foot in front of you and with your knee bent at 90 degrees. Raise your right hand over your head and tighten your right buttock to stretch your hip flexors. Push your pelvis forward and lean your torso to your left. Hold the stretch for five to six deeps breaths. Perform two sets of stretches on each side of your body.

Consult with a qualified health and exercise professional to determine the best strategy to address your lateral pelvic tilt condition. Since everyone has different bodies, health and causes of pain which lead to the lateral pelvic tilt, an exercise or method that works for one person may hurt another, says physical therapist MS SAIFI. Corrective exercise training for any condition must be based on each individual, never with a one-size-fits-all method.



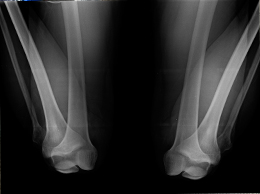
Previously‘’ Dr MS Saifi ’’has mentioned that our body is very flexible and move to do all type of work, so neither one posture is good or bad during work. But note it, that any strenuous posture, in which the muscles /ligaments work too much to hold that posture for long period, is not good. It may be dangerous for the joints and muscles, but it is too dangerous when one posture is repeated day to day and included in your habits. For example; cross leg sitting, knee band over the other leg, ‘’W’’ shape sitting & various strenuous knees postures. No one posture can implemented to all. It varies person to person or demands of work place. Excessive use of body or joints during exercise or daily activities can lead degenerative changes in the cartilage or osteoarthritis.
Mostly we feel pain when are in trouble. Whatever is the reason of injury? Medical professional diagnosed. The doctor may confirm the diagnosis by conducting a careful history and physical examination. Blood tests may be helpful for diagnosing rheumatoid arthritis, but other tests may also be needed. Analyzing fluid from the knee joint, for example, may be helpful in diagnosing gout. X rays may be taken to determine loss or damage to cartilage or bone.
Knee injuries can occur as the result of a direct blow or sudden movements that strain the knee beyond its normal range of motion. Sometimes knees are injured slowly over time. Problems with the hips or feet, for example, can cause you to walk awkwardly, which throw off the alignment of the knees and leads to damage. Knee problems can also be the result of a lifetime of normal wear and tear. Much like the treads on a tire, the joint simply wears out over time. This publication discusses some of the most common knee injuries.
There are many diseases and types of injuries that can affect the knee. These are some of the most common, along with their diagnoses and treatment.
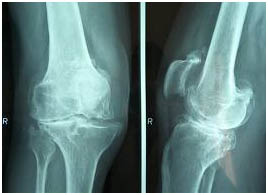
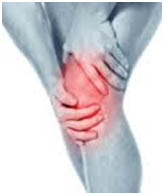
There are some 100 different forms of arthritis,1 rheumatic diseases, and related conditions. Virtually all of them have the potential to affect the knees in some way; however, the following are the most common.
The National Institute of Arthritis and Musculoskeletal and Skin Diseases Information Clearinghouse has separate publications on the different forms of arthritis mentioned in this section.
Some people with knee problems have a form of arthritis called osteoarthritis. In this disease, the cartilage gradually wears away and changes occur in the adjacent bone. Osteoarthritis may be caused by joint injury or being overweight. It is associated with aging and most typically begins in people age 50 or older. A young person who develops osteoarthritis typically has had an injury to the knee or may have an inherited form of the disease.
Rheumatoid arthritis, which generally affects people at a younger age than does osteoarthritis, is an autoimmune disease. This means it occurs as a result of the immune system attacking components of the body. In rheumatoid arthritis, the primary site of the immune system’s attack is the synovium, the membrane that lines the joint. This attack causes inflammation of the joint. It can lead to destruction of the cartilage and bone and, in some cases, muscles, tendons, and ligaments as well.
These include: Gout. An acute and intensely painful form of arthritis that occurs when crystals of the bodily waste product uric acid are deposited in the joints.
An autoimmune disease characterized by destructive inflammation of the skin, internal organs, and other body systems, as well as the joints.
An inflammatory form of arthritis that primarily affects the spine, leading to stiffening and in some cases fusing into a stooped position.
A condition in which inflamed joints produce symptoms of arthritis for patients who have or will develop psoriasis.
A term describing forms of arthritis that are caused by infectious agents, such as bacteria or viruses. Prompt medical attention is essential to treat the infection and minimize damage to joints, particularly if fever is present.
The symptoms are different for the different forms of arthritis. For example, people with rheumatoid arthritis, gout, or other inflammatory conditions may find the knee swollen, red, and even hot to the touch. Any form of arthritis can cause the knee to be painful and stiff.
The doctor may confirm the diagnosis by conducting a careful history and physical examination. Blood tests may be helpful for diagnosing rheumatoid arthritis, but other tests may also be needed. Analyzing fluid from the knee joint, for example, may be helpful in diagnosing gout. X rays may be taken to determine loss or damage to cartilage or bone.
People with any type of arthritis may benefit from exercises to strengthen the muscles that support the knee and from weight loss, if needed, to relieve excess stress on the joints.
Medications: People with diseases such as rheumatoid arthritis, ankylosing spondylitis, or psoriatic arthritis often require disease-modifying antirheumatic drugs (DMARDs) or biologic response modifiers (biologics) to control the underlying disease that is the source of their knee problems. These drugs are typically prescribed after less potent treatments, such as NSAIDs or intra-articular injections, are deemed ineffective.
Surgical treatment:If arthritis causes serious damage to a knee or there is incapacitating pain or loss of use of the knee from arthritis, joint surgery may be considered. Traditionally, this has been done with what is known as a total knee replacement. However, newer surgical procedures are continuously being developed that include resurfacing or replacing only the damaged cartilage surfaces while leaving the rest of the joint intact
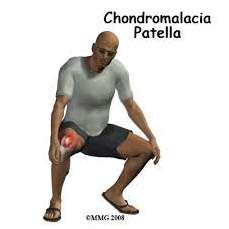
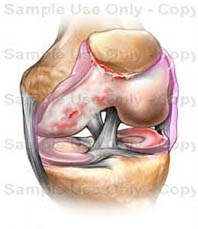
Chondromalacia (KON-dro-mah-LAY-she-ah), also called chondromalacia patellae, refers to softening of the articular cartilage of the kneecap. This disorder occurs most often in young adults and can be caused by injury, overuse, misalignment of the patella, or muscle weakness. Instead of gliding smoothly across the lower end of the thigh bone, the kneecap rubs against it, thereby roughening the cartilage underneath the kneecap. The damage may range from a slightly abnormal surface of the cartilage to a surface that has been worn away to the bone. Chondromalacia related to injury occurs when a blow to the kneecap tears off either a small piece of cartilage or a large fragment containing a piece of bone (osteochondral fracture).
The most frequent symptom of chondromalacia is a dull pain around or under the kneecap that worsens when walking, down stairs or hills. A person may also feel pain when climbing stairs or when the knee bears weight as it straightens. The disorder is common in runners and is also seen in skiers, cyclists, and soccer players.
Your description of symptoms and an x ray usually help the doctor make a diagnosis. Although arthroscopy can confirm the diagnosis, it’s not performed unless conservative treatment has failed.
Many doctors recommend that people with chondromalacia perform low-impact exercises that strengthen muscles, particularly muscles of the inner part of the quadriceps, without injuring joints. Swimming, riding a stationary bicycle, and using a cross-country ski machine are examples of good exercises for this condition. Electrical stimulation may also be used to strengthen the muscles.
Increasingly, doctors are using osteochondral grafting, in which a plug of bone and healthy cartilage is harvested from one area and transplanted to the injury site. Another relatively new technique is known as autologous chondrocyte implantation (ACI). It involves harvesting healthy cartilage cells, cultivating them in a lab, and implanting them over the lesion. If these treatments don’t improve the condition, the doctor may perform arthroscopic surgery to smooth the surface of the cartilage and “wash out” the cartilage fragments that cause the joint to catch during bending and straightening. In more severe cases, surgery may be necessary to correct the angle of the kneecap and relieve friction between it and the cartilage, or to reposition parts that are out of alignment.
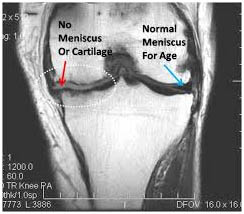
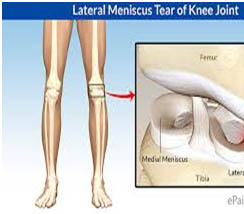
The menisci can be easily injured by the force of rotating the knee while bearing weight. A partial or total tear may occur when a person quickly twists or rotates the upper leg while the foot stays still (for example, when dribbling a basketball around an opponent or turning to hit a tennis ball). If the tear is tiny, the meniscus stays connected to the front and back of the knee; if the tear is large, the meniscus may be left hanging by a thread of cartilage. The seriousness of a tear depends on its location and extent
Generally, when people injure a meniscus, they feel some pain, particularly when the knee is straightened. If the pain is mild, the person may continue moving. Severe pain may occur if a fragment of the meniscus catches between the femur and the tibia. Swelling may occur soon after injury if there is damage to blood vessels. Swelling may also occur several hours later if there is inflammation of the joint lining (synovium). Sometimes, an injury that occurred in the past but was not treated becomes painful months or years later, particularly if the knee is injured a second time. After any injury, the knee may click, lock, feel weak, or give way. Although symptoms of meniscal injury may disappear on their own, they frequently persist or return and require treatment
In addition to listening to your description of the onset of pain and swelling, the doctor may perform a physical examination and take x rays of the knee. An MRI may be recommended to confirm the diagnosis. Occasionally, the doctor may use arthroscopy to help diagnose a meniscal tear.
If the tear is minor and the pain and other symptoms go away, the doctor may recommend a muscle-strengthening program. The following exercises are designed to build up the quadriceps and hamstring muscles and increase flexibility and strength after injury to the meniscus: Warming up the joint by riding a stationary bicycle, then straightening and raising the leg (but not straightening it too much). Extending the leg while sitting (a weight may be worn on the ankle for this exercise). Raising the leg while lying on the stomach. Exercising in a pool (walking as fast as possible in chest-deep water, performing small flutter kicks while holding onto the side of the pool, and raising each leg to 90 degrees in chest-deep water while pressing the back against the side of the pool). Before beginning any type of exercise program, consult your doctor or physical therapist to learn which exercises are appropriate for you and how to do them correctly, because doing the wrong exercise or exercising improperly can cause problems. A health care professional can also advise you on how to warm up safely and when to avoid exercising a joint affected by arthritis. If your lifestyle is limited by the symptoms or the problem, the doctor may perform arthroscopic or open surgery to see the extent of injury and to remove or repair the tear. Most young athletes are able to return to active sports after meniscus repair. Recovery after surgical repair takes several weeks. The best results of treatment for meniscal injury are achieved in people who do not show articular cartilage changes and who have an intact anterior cruciate ligament.
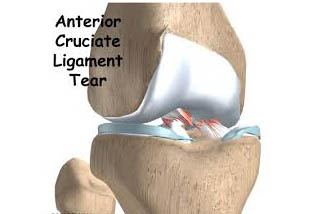
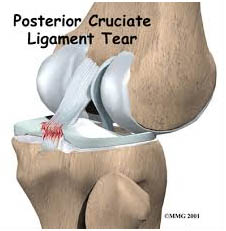
Cruciate ligament injuries are sometimes referred to as sprains. They don’t necessarily cause pain, but they are disabling. The anterior cruciate ligament is most often stretched or torn (or both) by a sudden twisting motion (for example, when the feet are planted one way and the knees are turned another). The posterior cruciate ligament is most often injured by a direct impact, such as in an automobile accident or football tackle.
You may hear a popping sound, and the leg may buckle when you try to stand on it.
The doctor may perform several tests to see whether the parts of the knee stay in proper position when pressure is applied in different directions. A thorough examination is essential. An MRI is accurate in detecting a complete tear, but arthroscopy may be the only reliable means of detecting a partial one.
For an incomplete tear, the doctor may recommend an exercise program to strengthen surrounding muscles. He or she may also prescribe a brace to protect the knee during activity. For a completely torn anterior cruciate ligament in an active athlete and motivated person, the doctor is likely to recommend surgery. The surgeon may reconstruct the torn ligament by using a piece (graft) of healthy tissue from you (autograft) or from a cadaver (allograft). Although synthetic ligaments have been tried in experiments, the results have not been as good as with human tissue. One of the most important elements in a successful recovery after cruciate ligament surgery is a 4- to 6-month exercise and rehabilitation program that may involve using special exercise equipment at a rehabilitation or sports center. Successful surgery and rehabilitation will allow the person to return to a normal lifestyle.
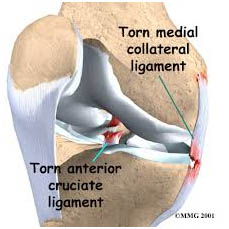
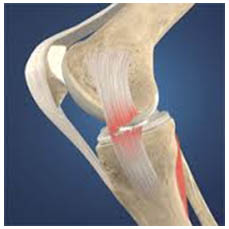
The medial collateral ligament is more easily injured than the lateral collateral ligament. The cause of collateral ligament injuries is most often a blow to the outer side of the knee that stretches and tears the ligament on the inner side of the knee. Such blows frequently occur in contact sports such as football or hockey.
When injury to the medial collateral ligament occurs, you may feel a pop and the knee may buckle sideways. Pain and swelling are common.
A thorough examination is needed to determine the type and extent of the injury. In diagnosing a collateral ligament injury, the doctor exerts pressure on the side of the knee to determine the degree of pain and the looseness of the joint. An MRI is helpful in diagnosing injuries to these ligaments.
Most sprains of the collateral ligaments will heal if you follow a prescribed exercise program. In addition to exercise, the doctor may recommend ice packs to reduce pain and swelling, and a small sleeve-type brace to protect and stabilize the knee. A sprain may take 2 to 4 weeks to heal. A severely sprained or torn collateral ligament may be accompanied by a torn anterior cruciate ligament, which usually requires surgical repair.
Knee tendon injuries range from tendinitis (inflammation of a tendon) to a ruptured (torn) tendon. If a person overuses a tendon during certain activities such as dancing, cycling, or running, the tendon stretches and becomes inflamed. Tendinitis of the patellar tendon is sometimes called “jumper’s knee” because in sports that require jumping, such as basketball, the muscle contraction and force of hitting the ground after a jump strain the tendon. After repeated stress, the tendon may become inflamed or tear.
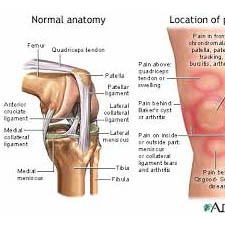
People with tendinitis often have tenderness at the point where the patellar tendon meets the bone. In addition, they may feel pain during running, hurried walking, or jumping. A complete rupture of the quadriceps or patellar tendon is not only painful, but also makes it difficult for a person to bend, extend, or lift the leg against gravity.
If there is not much swelling, the doctor will be able to feel a defect in the tendon near the tear during a physical examination. An x ray will show that the patella is lower than normal in a quadriceps tendon tear and higher than normal in a patellar tendon tear. The doctor may use an MRI to confirm a partial or total tear.
Initially, the treatment for tendinitis involves rest, elevating the knee, applying ice, and taking NSAID medications such as aspirin or ibuprofen to relieve pain and decrease inflammation and swelling. A series of rehabilitation exercises is also useful. If the quadriceps or patellar tendon is completely ruptured, a surgeon will reattach the ends. After surgery, a cast is worn for 3 to 6 weeks and crutches are used. For a partial tear, the doctor might apply a cast without performing surgery. Rehabilitating a partial or complete tear of a tendon requires an exercise program that is similar to but less vigorous than that prescribed for ligament injuries. The goals of exercise are to restore the ability to bend and straighten the knee and to strengthen the leg to prevent repeat injury. A rehabilitation program may last 6 months, although people can resume many activities before then.
Osgood-Schlatter disease is a condition caused by repetitive stress or tension on part of the growth area of the upper tibia (the apophysis). It is characterized by inflammation of the patellar tendon and surrounding soft tissues at the point where the tendon attaches to the tibia. The disease may also be associated with an injury in which the tendon is stretched so much that it tears away from the tibia and takes a fragment of bone with it. The disease most commonly affects active young people, particularly boys between the ages of 10 and 15, who play games or sports that include frequent running and jumping.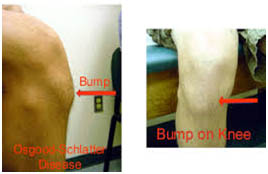
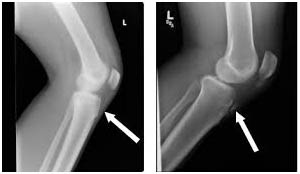
People with this disease experience pain just below the knee joint that usually worsens with activity and is relieved by rest. A bony bump that is particularly painful when pressed may appear on the upper edge of the tibia (below the kneecap). Usually, the motion of the knee is not affected. Pain may last a few months and may recur until the child’s growth is completed.
Osgood-Schlatter disease is most often diagnosed by the symptoms. An x ray may be normal, or show an injury, or, more typically, show that the growth area is in fragments.
Osgood-Schlatter disease is temporary and the pain usually goes away without treatment. Applying ice to the knee when pain begins helps relieve inflammation and is sometimes used along with stretching and strengthening exercises. The doctor may advise you to limit participation in vigorous sports. Children who wish to continue moderate or less stressful sports activities may need to wear knee pads for protection and apply ice to the knee after activity. If there is a great deal of pain, sports activities may be limited until the discomfort becomes tolerable.
Iliotibial band syndrome is an inflammatory condition caused when a band of tissue rubs over the outer bone (lateral condyle) of the knee. Although iliotibial band syndrome may be caused by direct injury to the knee, it is most often caused by the stress of long-term overuse, such as sometimes occurs in sports training and, particularly, in running.
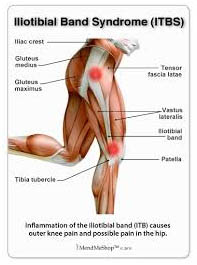
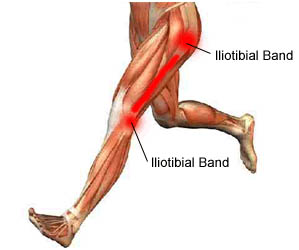
A person with this syndrome feels an ache or burning sensation at the side of the knee during activity. Pain may be localized at the side of the knee or radiate up the side of the thigh. A person may also feel a snap when the knee is bent and then straightened. Swelling is usually absent, and knee motion is normal.
The diagnosis of this disorder is typically based on the symptoms, such as pain at the outer bone, and exclusion of other conditions with similar symptoms.
Usually, iliotibial band syndrome disappears if the person reduces activity and performs stretching exercises followed by muscle-strengthening exercises. In rare cases when the syndrome doesn’t disappear, surgery may be necessary to split the tendon so it isn’t stretched too tightly over the bone.


Osteochondritis dissecans results from a loss of the blood supply to an area of bone underneath a joint surface. It usually involves the knee. The affected bone and its covering of cartilage gradually loosen and cause pain. This problem usually arises spontaneously in an active adolescent or young adult. It may be caused by a slight blockage of a small artery or to an unrecognized injury or tiny fracture that damages the overlying cartilage. A person with this condition may eventually develop osteoarthritis. Lack of a blood supply can cause bone to break down (osteonecrosis).5 The involvement of several joints or the appearance of osteochondritis dissecans in several family members may indicate that the disorder is inherited.
If normal healing doesn’t occur, cartilage separates from the diseased bone and a fragment breaks loose into the knee joint, causing weakness, sharp pain, and locking of the joint.
An x ray, MRI, or arthroscopy can determine the condition of the cartilage and can be used to diagnose osteochondritis dissecans.
If cartilage fragments have not broken loose, a surgeon may fix them in place with pins or screws that are sunk into the cartilage to stimulate a new blood supply. If fragments are loose, the surgeon may scrape down the cavity to reach fresh bone, add a bone graft, and fix the fragments in position. Fragments that cannot be mended are removed, and the cavity is drilled or scraped to stimulate new cartilage growth. Research is being done to assess the use of cartilage cell and other tissue transplants to treat this disorder.


Plica (PLI-kah) syndrome occurs when plicae (bands of synovial tissue) are irritated by overuse or injury. Synovial plicae are the remains of tissue pouches found in the early stages of fetal development. As the fetus develops, these pouches normally combine to form one large synovial cavity. If this process is incomplete, plicae remain as four folds or bands of synovial tissue within the knee. Injury, chronic overuse, or inflammatory conditions are associated with this syndrome.
Symptoms of plica syndrome include pain and swelling, a clicking sensation, and locking and weakness of the knee.
Because the symptoms are similar to those of some other knee problems, plica syndrome is often misdiagnosed. Diagnosis usually depends on excluding other conditions that cause similar symptoms.
The goal of treatment for plica syndrome is to reduce inflammation of the synovium and thickening of the plicae. The doctor usually prescribes medicine such as ibuprofen to reduce inflammation. People are also advised to reduce activity, apply ice and an elastic bandage to the knee, and do strengthening exercises. A cortisone injection into the plica folds helps about half of those treated. If treatment fails to relieve symptoms within 3 months, the doctor may recommend arthroscopic or open surgery to remove the plicae.
After an examination by your primary care doctor, he or she may refer you to a Rheumatologist, A rheumatologist specializes in nonsurgical treatment of arthritis Orthopedic surgeon, specializes in nonsurgical and surgical treatment of arthritis.
They may also be referred to Physiotherapis Specializing in physical medicine and rehabilitation, Physiotherapist seek to restore optimal function to people with injuries to the muscles, bones, tissues, and nervous system.
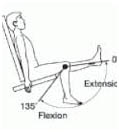
Range-of-motion exercises to help maintain normal joint movement and relieve stiffness.
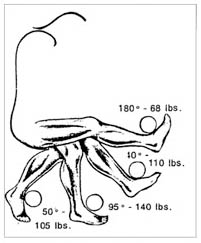
Strengthening exercises to help keep or increase muscle strength. Keeping muscles strong with exercises, such as walking up stairs, doing leg lifts or dips, or riding a stationary bicycle, helps support and protect the knee.
Aerobic or endurance exercises to improve function of the heart and circulation and to help control weight. Weight control can be important to people who have arthritis because extra weight puts pressure on many joints. Some studies show that aerobic exercise can reduce inflammation in some joints.

If you already have knee problems, your doctor or physical therapist can help with a plan of exercise that will help the knee(s) without increasing the risk of injury or further damage. As a general rule, you should choose gentle exercises such as swimming, aquatic exercise, or walking rather than jarring exercises such as jogging or high-impact aerobics.
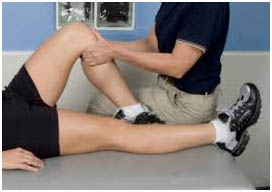
Some knee problems, such as those resulting from an accident, cannot be foreseen or prevented. However, people can prevent many knee problems by following these suggestions: Before exercising or participating in sports,warm up by walking or riding a stationary bicycle

stretches: Stretching the muscles in the front of the thigh (quadriceps) and back of the thigh (hamstrings) reduces tension on the tendons and relieves pressure on the knee during activity.

Strengthen: the leg muscles by doing specific exercises (for example, by walking up stairs or hills or by riding a stationary bicycle). A supervised workout with weights is another way to strengthen the leg muscles that support the knee. Avoid sudden changes in the intensity of exercise. Increase the force or duration of activity gradually.
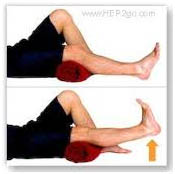

Wear shoes: that fit properly and are in good condition. This will help maintain balance and leg alignment when walking or running. Flat feet or over pronated feet (feet that roll inward) can cause knee problems. People can often reduce some of these problems by wearing special shoe inserts (orthotics). Maintain a healthy weight to reduce stress on the knee. Obesity increases the risk of osteoarthritis of the knee.
.jpg)
Wearing High heel, standing on the one leg , twisting the leg against the foot, poor shoes fitting ,poor standing posture, pathological/postural deformities of ankle/foot & physiological problems can lead ankle/forefoot pain & tend to bad posture.
Clubfoot (congenital talipes equinovarus) is a deformity that is present at birth in about one in every 1,000 children. It occurs in males more often than females, and can affect one or both feet. The feet of an infant with clubfoot point down and inward. It is not painful, but must be corrected to avoid a lifetime of disability. Parents can be assured that, in most cases, clubfoot can be effectively treated if it is undertaken as early as possible. Casting of the legs and feet is usually successful, but in some cases surgery may be required.
“Drop foot” refers to the inability to lift the front part of one’s foot off the ground when walking, resulting in a scuffing or dragging of the foot or lifting the thigh (known as “steppage” gait). It is most often caused by nerve or muscle disorders or damage, or by a central nervous system disorder. Drop foot is usually diagnosed by physical examination, although additional testing may be recommended in some cases. Treatment may include use of braces, physical therapy, and electrical nerve stimulation. In some cases surgery may be required.
If you have a bunion, you know it can be a painful enlargement at the joint of the big toe. The skin over the joint becomes swollen and is often quite tender. Bunions can be inherited as a family trait, can develop with no recognizable cause or can be caused by shoes that fit poorly. An important part of treatment is wearing shoes that conform to the shape of the foot and do not cause pressure areas. This often alleviates the pain. In severe cases, bunions can be disabling. Several types of surgery are available that may relieve pain and improve the appearance of the foot. Surgery is usually done to relieve pain and is not meant for cosmetic purposes.
Heel pain is extremely common. It often begins without injury and is felt under the heel, usually while standing or walking. It is usually worst when arising out of bed. Inflammation of the connective tissue on the sole of the foot (plantar fascia) where it attaches to the heel bone is the most common cause of pain. It is often associated with a bony protrusion (heel spur) seen on X-ray studies.
Most cases of heel pain will improve with physiotherapy . ULTRASONIC massage, TENS, THERMOTHERAPY OR CRYOTHERAPY MAY HELP TO REDUCE Heel and stretching PAIN. Medication to reduce swelling of the soft tissues in your foot and shoe inserts are quite helpful. If pain continues, steroid injections or walking casts are used. Only in the most troubling and prolonged cases is surgery recommended.
Morton’s neuroma is caused by a nerve being pinched. This pinching usually results in pain between the third and fourth toes. Tight shoes can squeeze foot bones together. The nerve responds by forming a neuroma, a build up of extra tissue in the nerve. The neuroma results in pain, that may radiate into the toes. Treatment usually involves wearing wider shoes and taking oral medications to decrease the swelling around the nerve. A pad on the sole of the foot to spread the bones is often helpful. Your doctor may also inject cortisone around the nerve. If your difficulty continues, surgery to remove the neuroma may be suggested. Physiotherapist can help to reduce pain using electrotherapy.
Corns and calluses are caused by pressure on the skin of your foot. They may occur when bones of the foot press against the shoe or when two foot bones press together. Common sites for corns and calluses are on the big toe and the fifth toe. Calluses underneath the ends of the foot bones (metatarsals) are common. Soft corns can occur between the toes.
Treatment involves relieving the pressure on the skin, usually by modifying the shoe. Pads to relieve the bony pressure are helpful, but they must be positioned carefully. On occasion, surgery is necessary to remove a bony prominence that causes the corn or callus.
Hammertoes are one of several types of toe deformities. Hammertoes have a permanent sideways bend in your middle toe joint. The resulting deformity can be aggravated by tight shoes and usually results in pain over the prominent bony areas on the top of the toe and at the end of the toe. A hard corn may develop over this prominence. Treatment usually involves a shoe to better accommodate your deformed toe. Shoe inserts or pads also may help. If, after trying these treatments, you are still having marked difficulty, surgical treatment to straighten the toe or remove the prominent area of bone may be necessary.
Plantar warts occur on the sole of the foot and look like calluses. They result from an infection by a specific virus. They are like warts elsewhere, but they grow inward. The wart cannot grow outward because of weight placed on it when you stand. You may experience severe pain when walking, and can have just one or many plantar warts. Plantar warts are extremely difficult to treat, but success has been achieved with repeated applications of salicylic acid (available over the counter) to soften the overlying callus and expose the virus. Other treatments include injection of the warts with medication, freezing the warts with liquid nitrogen and, very rarely, surgery.
Achilles tendonitis is an inflammation of the Achilles tendon. This inflammation is typically short-lived. Over time, if not resolved, the condition may progress to a degeneration of the tendon (Achilles tendonosis), in which the tendon loses its organized structure and is likely to develop microscopic tears. Sometimes the degeneration involves the site where the Achilles tendon attaches to the heel bone. In rare cases, chronic degeneration with or without pain may result in rupture of the tendon.
As “overuse” disorders, Achilles tendonitis and tendonosis are usually caused by a sudden increase of a repetitive activity involving the Achilles tendon. Such activity puts too much stress on the tendon too quickly, leading to micro-injury of the tendon fibers. Due to this ongoing stress on the tendon, the body is unable to repair the injured tissue. The structure of the tendon is then altered, resulting in continued pain.
Athletes are at high risk for developing disorders of the Achilles tendon. Achilles tendonitis and tendonosis are also common in individuals whose work puts stress on their ankles and feet, such as laborers, as well as in “weekend warriors”—those who are less conditioned and participate in athletics only on weekends or infrequently.
Treatment approaches for Achilles tendonitis or tendonosis are selected on the basis of how long the injury has been present and the degree of damage to the tendon. In the early stage, when there is sudden (acute) inflammation, one or more of the following options may be recommended:
Non steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, may be helpful in reducing the pain and inflammation in the early stage of the condition.
If non-surgical approaches fail to restore the tendon to its normal condition, surgery may be necessary. The foot and ankle surgeon will select the best procedure to repair the tendon, based upon the extent of the injury, the patient’s age and activity level, and other factors.
To prevent Achilles tendonitis or tendonosis from recurring after surgical or non-surgical treatment, the foot and ankle surgeon may recommend strengthening and stretching of the calf muscles through daily exercises. Wearing proper shoes for the foot type and activity is also important in preventing recurrence of the condition.
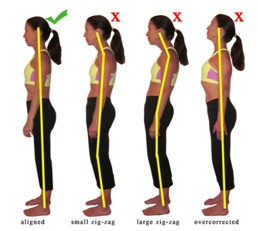
find out how everyday standing and sitting habits can cause back pain and other ailments. common posture mistakes and how to correct them with strength and stretching exercises. "Correcting your posture may feel awkward at first because your body has grown so used to sitting and standing incorrectly," "You need to retrain your body to sit and stand correctly. Initially, this may require a bit of conscious effort and some strengthening and flexibility exercises to correct muscle imbalances.

If your bottom tends to stick out or you have a increased curve in your lower back, you may have "hyperlordosis", which is an exaggerated inward curve in the lower back creating a "Donald Duck" posture. This is often caused by tightness in your lower back and hip flexors and weakness in your core muscles, hamstrings and buttocks. These muscle imbalances tilt your pelvis forward and can cause lower back stiffness and pain. Wearing high heels, excessive weight around the stomach and pregnancy can all cause this posture. Core and buttock strengthening exercises and hip flexor and thigh stretches are recommended to help correct a sticking out bottom.

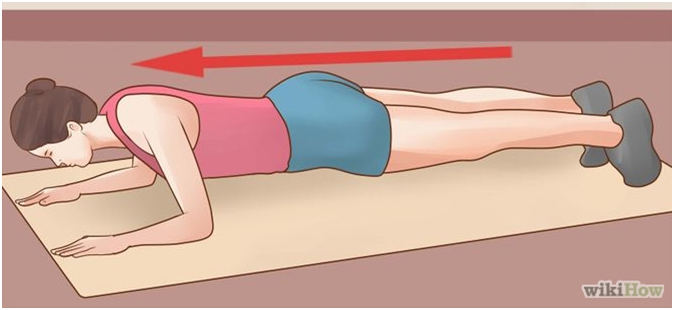
Lie on your front propped up on your forearms and toes. Keep your legs straight and hips raised to create a straight and rigid line from head to toe. Your shoulders should be directly above your elbows. Focus on keeping your abs contracted during the exercise. Hold this position for 5 to 10 seconds and repeat 8 to 10 times.

Lie on your side propped up on an elbow. Your shoulder should be directly above your elbow. Straighten your legs and raise your hips to create a straight and rigid line from head to toe. Keep your neck long and shoulders down and away from your ears. Keep your abs contracted during the exercise. Hold this position for 5 to 10 seconds and repeat 8 to 10 times. Repeat exercise on the other side.

Lie on your right side with your right knee bent at 90 degrees and your left leg straight and in line with your back. Press your left fingers into the top of your buttock to keep your left hip slightly tilting forward. Raise your left leg as far as you can without letting your hips tilt back. Slowly lower to starting position. Perform 8 to 10 times and repeat on the other side.
To help you maintain a correct standing posture, imagine a string attached to the top of your head pulling you upwards. The idea is to keep your body in perfect alignment, maintaining the spine's natural curvature, neck straight and shoulders parallel with the hips.

A flat back means your pelvis is tucked in and your lower back is straight instead of naturally curved, causing you to stoop forward. People with a flat back often find it difficult standing for long periods and can experience pain in the lower half of their back. This posture is often caused by muscle imbalances, which encourage you to adopt such a position. Spending long periods sitting down can also contribute to a flat back. A flat back may be a sign of tightness in your core and hamstrings, and weakness in your quadriceps, lower back and buttocks. A flat back also tends to make you lean your neck and head forwards, which can cause neck and upper back strain and pain. Exercises to strengthen your core, buttocks, neck and rear shoulder muscles and back extensions are recommended to help correct a flat back. Exercises to correct a flat back:

Leaning more on one leg while standing, sometimes referred to as "hanging on one hip", can feel comfortable, especially if you’ve been standing for a while, but it's often the result of weakness in some muscles. Instead of using your buttocks and core muscles to keep you upright, you place excessive pressure on one side of your lower back and hip. Over time, you may develop muscle imbalances around the pelvis area, which can cause muscular strain and pain in the lower back and buttocks. Other causes of uneven hips include carrying heavy backpacks on one shoulder, and mums carrying toddlers on one hip.
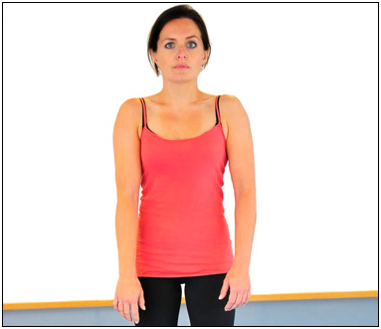
One way to tell if you've got rounded shoulders is to stand in front of a mirror and let your arms hang naturally by your sides. If your knuckles face forward, it may indicate that you have a tight chest and a weak upper back, giving the appearance of rounded shoulders, also called "upper cross syndrome". Rounded shoulders are typically caused by poor posture habits, muscle imbalances and an uneven exercise regimen, such as too much focus on chest strength and neglecting the upper back. Over time, these muscle imbalances will result in poor positioning of your shoulders, which can lead to shoulder and neck stiffness and pain.

"Poshitis" is the term coined for pain caused by the trend of carrying heavy handbags on a bent forearm as seen on fashionistas such as Victoria Beckham. Whether it’s handbags, backpacks, school bags or shopping bags, the way you carry your bag can wreak havoc on your posture and cause injury. Try this test: look in front of a mirror: are your shoulders level or tilting? If they tilt to one side, could this be due to always carrying a heavy load on the same shoulder? The best bags are empty ones. Carrying heavy bags improperly can stretch supporting muscles and ligaments, which can affect the back and shoulder alignment which in turn can cause posture-related stiffness and pain. Children are especially vulnerable to injury from carrying heavy bags, such as school bags, as their spines are still developing.


It's instinctive and feels natural, but sitting with your legs crossed puts pressure on your lower back. In this position, your hip tucks in, making it difficult to sit up straight, causing you to slouch. Over time you may develop muscle imbalances in your hips, which can cause stiffness and pain in the hips and lower back. Habits of a lifetime are hard to shake but for your back's sake, uncross those legs and sit up straight! It might feel awkward at first, but over time it will become second nature and your back will thank you for it.

Holding your phone handset between your ear and shoulder places undue stress on the muscles of the neck, upper back and shoulder. If you always cradle the phone on the same side, it may shorten, compress and weaken the neck muscles on one side while stretching the muscles on the opposite side. The neck and shoulders are not designed to hold this position for any length of time. This posture places strain on the muscles and other soft tissues leading to muscle imbalances between the left and right side of your neck, which can cause headaches and stiffness and pain in the neck, shoulders and arms. Try to get into the habit of holding the phone with your hand or use a hands-free device.
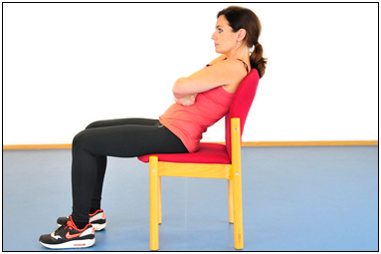
Sitting slumped without any lower back support may feel more comfortable than sitting upright because it requires less effort from our muscles, but it places a lot of pressure on your lower back. The reason you may slouch in the first place could be because you already have weak core muscles. In this posture, your pelvis is tucked in, instead of being level, leaving your lower back to support the weight of your upper body. The muscles that should be propping you up are dormant, putting strain on your ligaments, joints and other soft tissue structures of the lower back. In this position, your upper back will also have a tendency to hunch, creating its own problems (described in the hunched back section above). Get into the habit of sitting correctly. It may not feel comfortable initially because your muscles have not been conditioned to support you in the correct position. Exercises to strengthen your core and buttock muscles and back extensions will help correct a slouching posture.

The bridge exercise is a great way to isolate and strengthen the gluteus (butt) muscles and hamstrings (back of the upper leg). If you do this exercise correctly, you also will find that it is a good core stability and strengthening exercise that targets the abdominal muscles as well as the muscles of lower back and hip. Finally, the bridge exercise is considered a basic rehab exercise to improve core and spinal stabilization
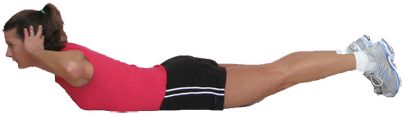
The above exercises featured moves targeting the lats, the largest muscles in the back. The back extension is a more subtle movement targeting the lower back. Many of us work our abs, but neglect to work the lower back, which can lead to muscle weakness and imbalance. Lie face down on a mat and place the hands on the floor or behind the head (more advanced).Contract the abs and keep them contracted throughout the exercise. Squeeze the back to lift the chest a few inches off the floor.Lower and repeat for 1-3 sets of 10-16 reps total on each arm.

If you work in an office and use a computer, you can avoid injury by sitting in the right position and arranging your desk correctly.
Avoid back pain by adjusting your chair so that your lower back is properly supported. A correctly adjusted chair will reduce the strain on your back. Get one that is easily adjustable so that you can change the height, back position and tilt. Have your knees level with your hips. You may need a footrest for this.
Adjust your chair height so that you can use the keyboard with your wrists and forearms straight and level with the floor. This can help prevent repetitive strain injuries. Your elbows should be by the side of your body so that the arm forms an L-shape at the elbow joint.
Your feet should be flat on the floor. If they’re not, ask if you can have a footrest, which lets you rest your feet at a level that’s comfortable. Don't cross your legs, as this can cause posture-related problems.
Your screen should be directly in front of you. A good guide is to place the monitor about an arm's length away, with the top of the screen roughly at eye level. To achieve this you may need to get a stand for your monitor. If the screen is too high or too low, you'll have to bend your neck, which can be uncomfortable.
Place your keyboard in front of you when typing. Leave a gap of about four to six inches (100mm-150mm) at the front of the desk to rest your wrists between bouts of typing. Your wrists should be straight when using a keyboard. Keep your elbows vertical under your shoulder and right by your side. Some people like to use a wrist rest to keep their wrists straight and at the same level as the keys.
Position and use the mouse as close to you as possible. A mouse mat with a wrist pad may help to keep your wrist straight and avoid awkward bending. If you are not using your keyboard, push it to one side if using the mouse a lot.
Your screen should be as glare-free as possible. If there’s glare on your screen, hold a mirror in front of it to identify the cause. Position the monitor to avoid reflection from overhead lighting and sunlight. If necessary, pull blinds across the windows and replace ceiling lighting with table lights. Adjusting the screen's brightness or contrast can make it much easier to use.
People with bifocal spectacles may find them less than ideal for computer work. It's important to be able to see the screen easily without having to raise or lower your head. If you can’t work comfortably with bifocals, you may need a different type of spectacles. Consult your optician if in doubt.
Position frequently used objects, such as your telephone or stapler, within easy reach. Avoid repeatedly stretching or twisting to reach things.
If you spend a lot of time on the phone, try exchanging your handset for a headset. Repeatedly cradling the phone between your ear and shoulder can strain the muscles in your neck.

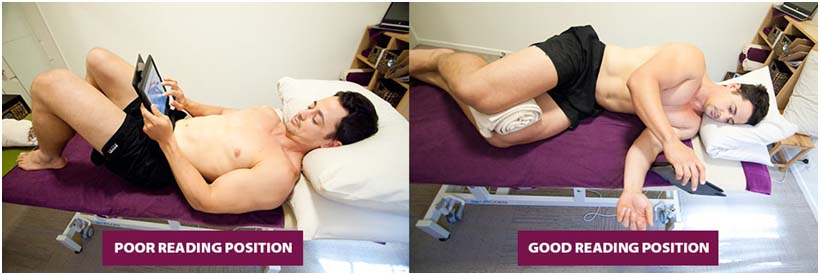
Finding the ideal sleep position for YOU is important to ensure that you don’t put any strain on your muscles and joints at night, especially if you already have a musculoskeletal condition. Some clients report to us that they feel stiff or painful first thing in the morning. This makes it extremely important for you to know if you are sleeping in the right position for your body.
One thing to note is that there is not one perfect pillow or mattress for everyone. We all have a different width of our shoulders and a different length of our spine. So how do you know what’s right?
Your muscles will tell you how happy your body is to be in the position you are in (this applies to other postures as well). The first thing to do is lay on your bed with your normal pillow in your usual sleep position. Place one or both of your hands on your neck muscles and move them around. Do the muscles feel squishy and relaxed, or do they feel tense and ropey? (Try to avoid pushing too hard with your fingers).

If your neck feels squishy and relaxed, then that pillow and that position is right for you. If your neck feels tense and ropey, you may need to adjust a few things. First assess this; Is your head in line with your neck, or is it Being pushed up too high, or Hanging down onto the pillow.
If your head is being pushed up high, the pillow may be too high for you. Try a different pillow, or if it is an orthopedic pillow that has a high side and a low side, try the low side. Once you have changed this, re-assess the muscles for squishy-neck

If your head is hanging down onto the pillow it may be too low for you. You could try a different pillow at home that is higher, or build up the height of the one you have. An easy way to build up height is to fold a towel and place it under the pillow. You may have to try different amounts of fold to get the perfect height for you. To keep the towel in place, put it inside your pillow case on the bottom side of the pillow. Then, re-assess your muscles for feeling soft & squishy.
If neither of these works, it may be worth trying a new pillow altogether and do the same tests with a new/different pillow. You can usually do this in store if you are purchasing a new one.

It is often best to avoid sleeping on your tummy for long periods of time as this position often builds up strain in your neck and/or shoulders. Try to make a habit out of sleeping on your back or side.
We will do a similar test on your low back muscles either side of your spine. Get into your usual comfortable position. If this is on your side, feel the top side of your back muscles. Do they feel squishy and relaxed, or do they feel tense and ropey.

If your low back muscles feel tense and ropey when you are on your side, try putting a pillow in between your knees and have your knees slightly bent. Re-assess your back muscles to see if that makes them more relaxed.
1 Similar to finding the right height pillow for you neck, you may have to do the same test/re-test for the pillow in between your knees
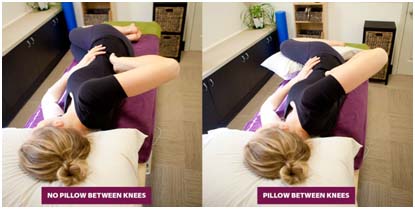
2 If you sleep on your back, slide your fingers under your back and feel the muscles either side of your spine. If they are tense, try putting a pillow under your knees.
If neither of these work, try pillows in different places on the bed to support yourself, especially if you are in pain.




A housewife is a woman whose main occupation is running or managing her family's home—caring for and educating her children, cooking and storing food, buying goods the family needs in day-to-day life, cleaning and maintaining the home, making clothes for the family, etc.—and who is generally not employed outside the home. While modern homemakers in western nations may participate in a huge variety of activities, the traditional job of a housewife is to take care of her spouse and other members of the household and participate in the care of their home. Some of the traditional things that a housewife does are: Child care (where applicable) Cleaning, decorating and provision of clothing ,Doing first aid, Caring for sick people, Caring for pets (feeding, veterinarian visits, etc.), Listening to people's stories of their day, Entertaining guests and hosting parties and gatherings, Fixing things that go wrong, Finding lost things. Feeding babies and young children. Because of all day activities with forward bending posture get pain to the neck, back, knees, fibromyalgia, or fatigue easily ADVICE. Don’t do strenuous activity for prolong time. Maintain position during household


This would NOT be the proper posture at work, but we see it everyday. Many of my patients complain of pain at work and their job activities is one thing that increases their pain. One simple adjustment, away for the desk, is to avoid poor lifting technique and repetitive lifting. This can predispose you to low back pain. Also try to avoid prolonged awkward postures, below the waist or overhead lifting, trunk twisting, and excessive reaching.
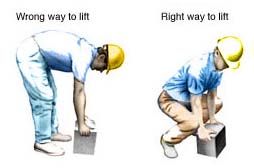
To lift a very light object from the floor, such as a piece of paper, lean over the object, slightly bend one knee and extend the other leg behind you. Hold on to a nearby chair or table for support as you reach down to the object.

Whether you are lifting a heavy laundry basket or a heavy box in your garage, remember to get close to the object, bend at the knees, and lift with your leg muscles. Do not bend at your waist.
When lifting luggage, stand alongside of the luggage, bend at your knees, grasp the handle and straighten up.

While you are holding the object, keep your knees slightly bent to maintain your balance. If you have to move the object to one side, avoid twisting your body. Point your toes in the direction you want to move and pivot in that direction. Keep the object close to you when moving.


If you must place an object on a shelf, move as close as possible to the shelf. Spread your feet in a wide stance, positioning one foot in front of the other to give you a solid base of support. Do not lean forward and do not fully extend your arms while holding the object in your hands. If the shelf is chest high, move close to the shelf and place your feet apart and one foot forward. Lift the object chest high, keep your elbows at your side and position your hands so you can push the object up and on to the shelf. Remember to tighten your stomach muscles before lifting.
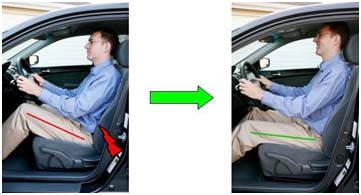
The ergonomics of your car’s command centre, the driver’s seat, is the most important thing you need to get right in order to avoid discomfort and fatigue while driving.
Luckily the car companies have already done a lot of work to make it easy for you to get it just about perfect. Unfortunately the vast majority of people don’t know how to properly adjust the driver’s seat.
The lumbar support can be a saving grace during long drives, or if you already suffer from back pain. If your car seat does not have an integrated lumbar support you should get an after market one.
Adjust the lumbar support so that the curve of your spine is evenly supported. Make sure not to over do it. You don’t want your S-curve being pushed out. Just a nice, gentle, even support.


To avoid pain in your neck, arms, and back during your motorcycle ride, it is important to have proper body posture. As a physiotherapist, I am concerned about fellow riders and their posture.
In my experience, many cyclists are riding bikes that are too big for them and many cyclists lack proper flexibility and/or their core strength is lacking. Take the time and have your bike fitted to your body. Also, back pain can arise from anatomical causes like leg length discrepancy or misalignment of your spine.
So much of what cyclists do is hunching forward—working on computers, riding bicycles, eating at dinner tables all contribute to bad spinal health. Poor spinal health is common in young cyclists and often due to bad posture (on and off the bike) and injury. If you favor one side of your body or the other due to injury or poor posture, your back eventually takes the strain. An imbalance in the spine will cause overuse of the lower back.
There are three basic postures while riding a motorcycle. Each posture has variability based on the bike design and size of the operator. The basic postures are Standard, Sport, and Cruiser. Each has it’s pros and cons.

Notice how Susan has a neutral upright position to her lower back and pelvis. Her arms and shoulders are relaxed and she can reach all the controls. This posture is very neutral. It keeps the back straight and the neck in a more neutral posture. The shoulders and elbows are held comfortably on the grips without over reaching or over-extending the elbows. Elbow are flexed, and forearms are parallel to the ground.
It is important that the shoulders be neutral. If you have a small frame or you are riding a bike that is too big, the controls may be slightly out of reach for you. This will cause you to lean forward or, worse, over-reach in order to gain access to the controls. Prolonged over-reached posture can lead to shoulder injuries such as trigger points, thoracic outlet syndrome, and shoulder impingement syndrome.

Susan's sport bike posture shows us the forward lean and forward tilt of the pelvis. Notice how the head is in slight extension. Sport posture looks fun and exciting but it can have the trauma on the body. In the sport posture, the body is in a forward lean, the feet are typically behind the knees, head is in extension. The forearms ought to be parallel to the ground. The wrists should be close to neutral.
At higher speeds, the weight of the body is supported by air pressure rushing onto the torso. But at low speeds there is not enough pressure and the operator is supporting his upper body weight on the wrists, and by extending the lower spinal posture muscles. Also the muscles in the top of the neck are supporting the head, which can lead to suboccipital headaches. This posture can lead to injury in the wrists, creating ligament inflammation and nerve compression, like carpal tunnel syndrome, as well as strain to the muscles in the neck and lower back. The nice thing is, the wind pressure keeps the upper body well balanced and the spinal muscles are less likely to fatigue.
The streets in St George UT are not built for sport bike posture. Our speed limits are quite low (30-40mph), and it is tough to get enough air pressure to support the upper body. Thankfully, the roads are well maintained so the bike operator does not have to deal with additional pressure injury on the wrists from bouncing through pot-holes.
This posture has the pelvis in extension, which can aggravate certain types of disc injuries.

Cruiser posture has the feet forward, low-slung seat, and slightly higher grips and controls. This posture has the operator is a slightly reclined position. The feet are often forward relative to the knee. The grips and controls are slightly higher. The head is upright and neutral. The hips and pelvis are relaxed, with the legs held close to the fuel tank.
This posture looks and feels comfortable, especially for older riders, and at lower speeds. With the pelvis in a minimal flexed posture, there is decreased sacral base angle pressure on the L5-S1 inter vertebral disc.
At higher speeds, riding without a fairing causes a huge increase in air pressure on the riders chest. As a result, the rider must lean slightly forward to maintain appropriate grip on the controls. This can cause some fatigue issues for the muscles on the front of the neck and abdomen.
Whatever your preferred riding posture might be, make sure you are taking appropriate steps to stay healthy as well as safe. Remember to hold the wrists, shoulders, neck and low-back in proper alignment. Doing so will not only reduce your risk of muscle fatigue, but it makes you a safer rider. If you are having pain associated with your ride, then stop by our physiotherapy centre and let us fix you up so you can enjoy your life with out pain.
Copyright @ 2025 Dr Saifi's Physiotherapy centre.All Rights Reserved. Designed By Official Solutions